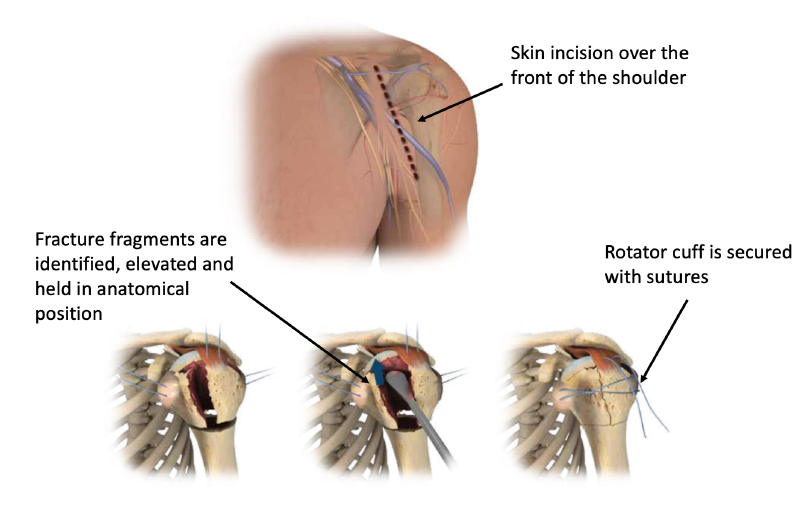
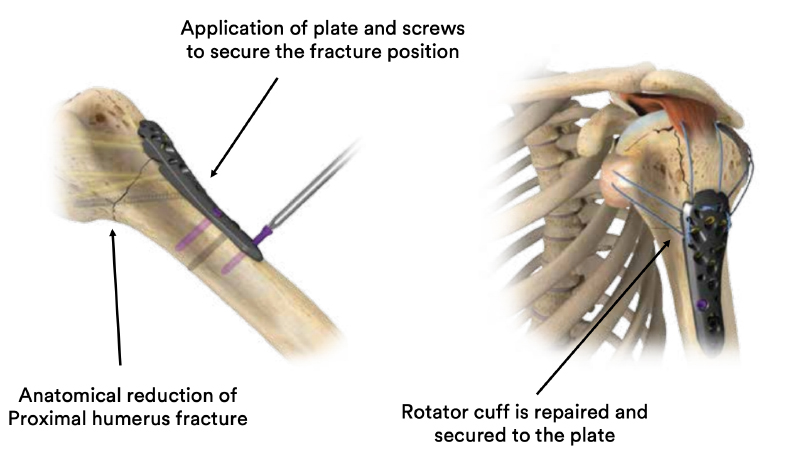
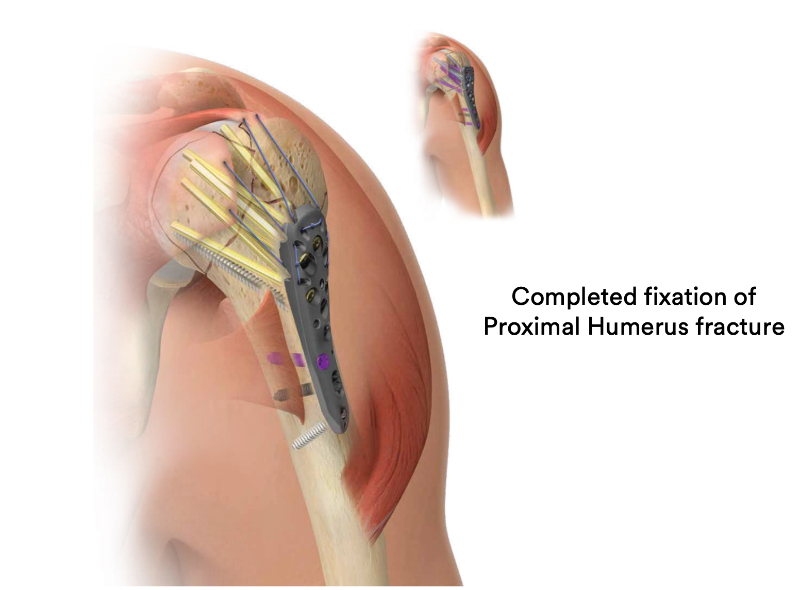
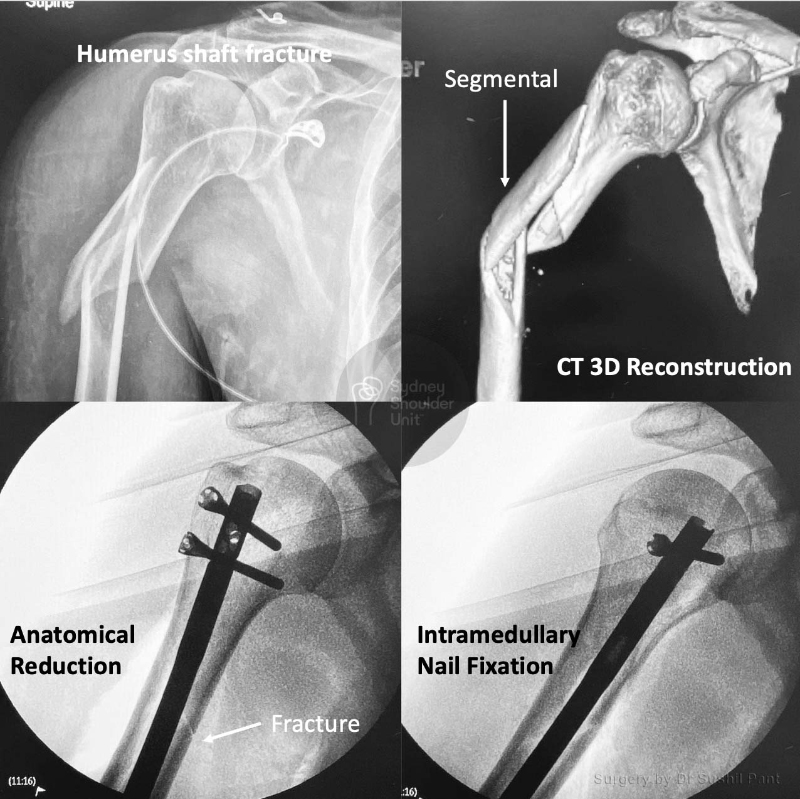
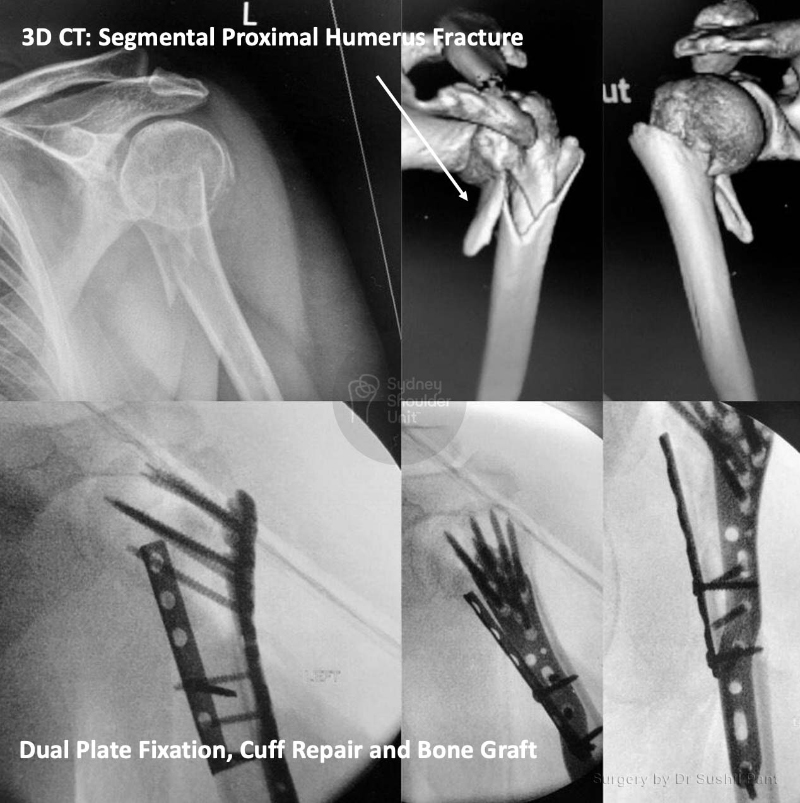
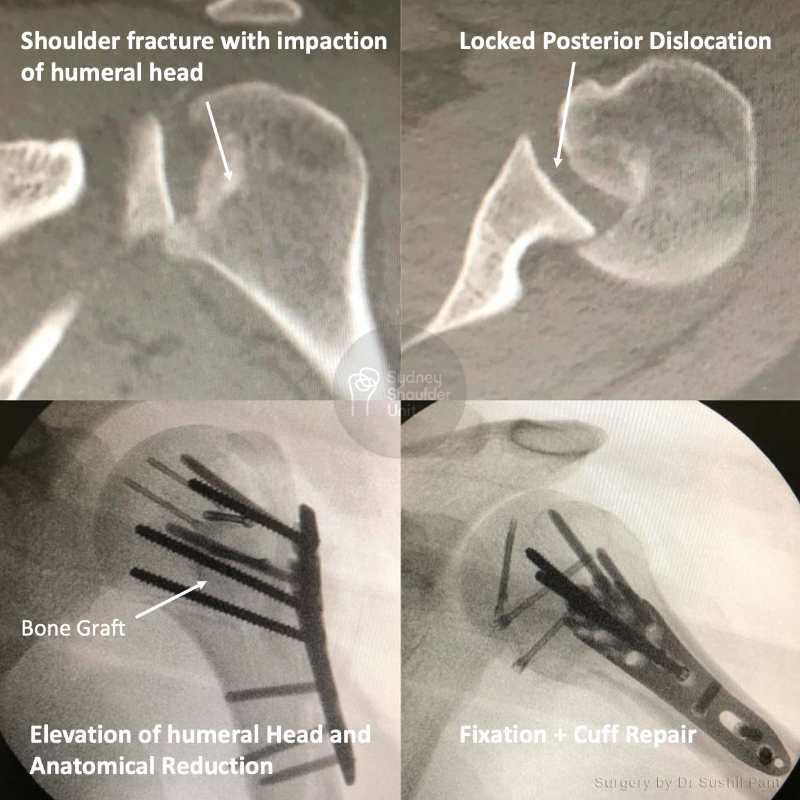
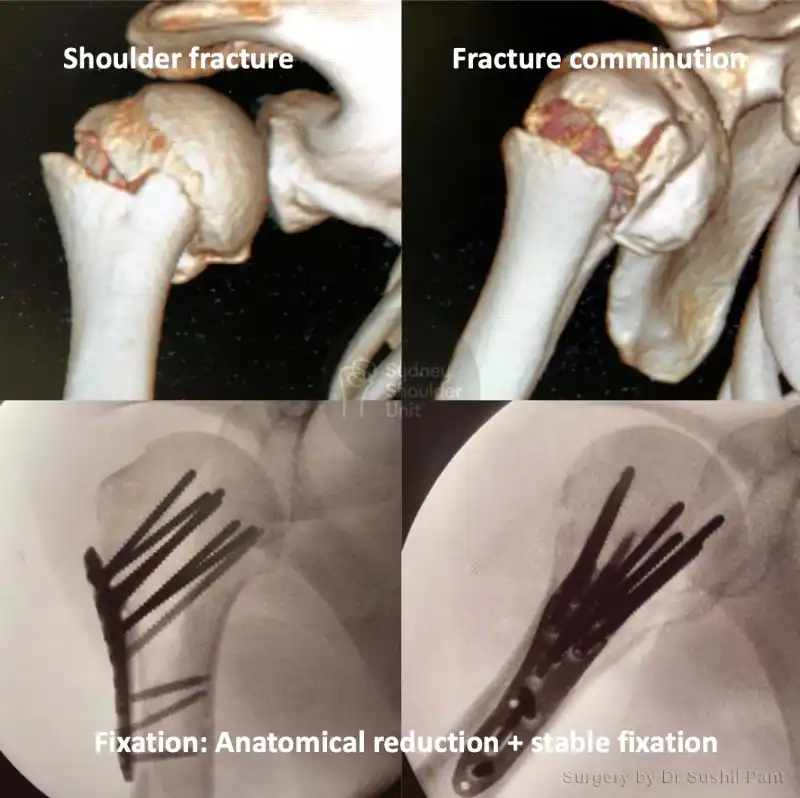
Most patients report a sense of “relief” after their proximal humerus fracture is fixed and can commence light activity with the operated arm (such as self care, feeding, and using a mobile phone) immediately.
There are three essential components to a good outcome from surgery:
- Your surgeon
- You as a patient
- Your physiotherapist
Post-operative physiotherapy
Dr Pant utilises the JPL pathway for most patients and this will form the basis of your rehabilitation after surgery; it will be modified to suit your individual circumstance.
The JPL pathway allows for self-directed, early passive shoulder range of movement:
- Passive = assisted with your other arm
- Active = you move the affected arm independently
Either a “standard” or an “abduction” sling is required for the first 6 weeks after your surgery. A “standard” sling is worn for a further 6 weeks outside of the house (to remind others you have had shoulder surgery). The type of sling is selected specific to you and your shoulder surgery.
Therapy overview
After the surgery you will be in a sling and protect your shoulder to allow the shoulder fracture repair to heal. At two weeks after the surgery Dr Pant will see you at your review appointment and discuss the JPL rehabilitation protocol with you. This JPL physiotherapy protocol will commence two weeks after your surgery.
The therapy program will focus on flexibility and range of motion exercises initially. These gentle stretches will improve your range of motion and prevent shoulder stiffness. As the fracture begins to heal you will be able to progress to exercises that strengthen your shoulder muscles. Shoulder and rotator cuff strengthening exercises are commenced at 12 weeks after shoulder fracture surgery. Dr Pant will discuss when it is safe to return to your chosen sports. Generally, collision sports and overhead contact athletes need more time to allow for healing.
Driving after proximal humerus fracture surgery
- After shoulder surgery, you will be in a sling and you may be unable to drive for at least 6-8 weeks
Showering and getting dressed
- You may take the sling off to shower
- Lean forward and allow your arm to “dangle” to wash under your arms
- The dressings applied are waterproof and you may shower with them on
- Usually, before you are discharged from Hospital, your dressings are changed after your morning shower.
- These “new” dressings are then kept intact until your review at 10-14 days
- If the dressings start to peel at the edges – you may reinforce them
- If the dressings discolour with discharge (yellow or green) you may have a wound infection – Do not be concerned just yet; please notify SSU (02 9215 6100 or admin@drpant.com.au) and we will give you a plan.
- When getting dressed, you may use your good arm to move your affected (operated arm) to place your arms through the sleeves carefully
Sleeping after Shoulder Surgery
- Most patients find it difficult to lie flat after shoulder surgery (especially after an ORIF Proximal Humerus)
- Consider using a few pillows to prop yourself up and sleep at a slight incline; this may be necessary for 4-6 weeks after surgery. You should keep your sling on while asleep.
Elbow and hand movement
- Keep your elbow and hands joints moving and supple for the duration of time you are in the sling
- The best time to move your elbow (into full extension and flexion) is when you are in the shower, just out of the shower and about to get dressed.