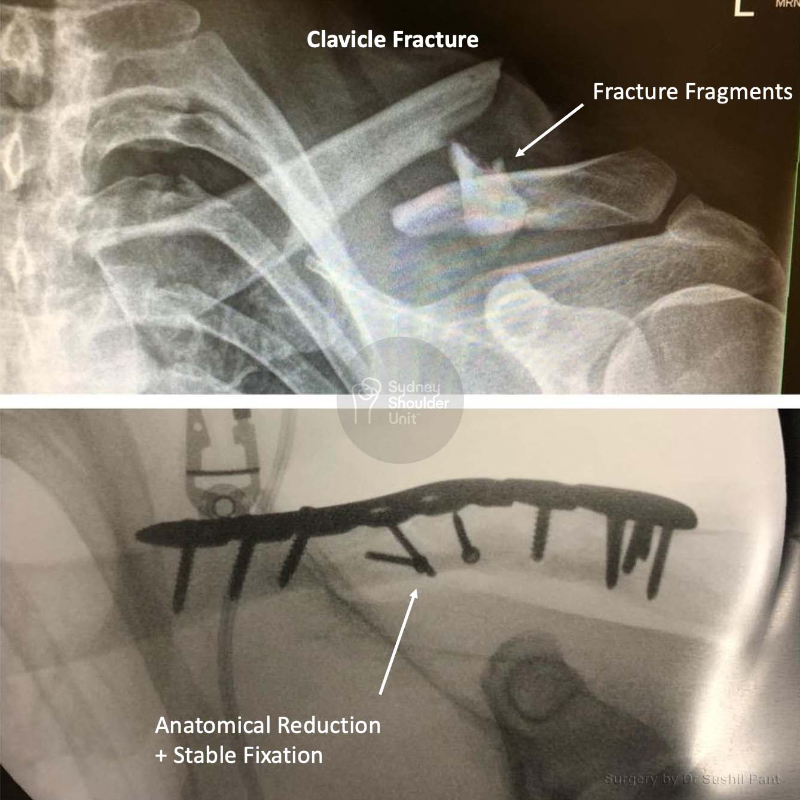
In some cases surgery is a better option; the factors to consider are:
- Displacement (fracture fragments further away)
- Comminution (how many parts the fracture is in)
- Other injuries (about the shoulder or elsewhere)
- Occupation (overhead, heavy lifting, manual work etc)
- Sporting demands
- Pain management
- Social situation
The decision to proceed with surgery is unique to each individual and based on their clavicle fracture pattern, social/work circumstances and expectations.
Dr Pant has extensive experience treating clavicle fractures and is highly skilled in the surgical repair of all clavicle fractures should that be required. As the lead shoulder trauma surgeon at St Vincent’s Hospital for many years, he has come to deal with a vast array of shoulder trauma cases and is well versed in guiding you to full recovery.
At Sydney Shoulder Unit we treat many types of clavicle fractures and keep aside “priority” appointment slots for an urgent review of patients who have sustained a fracture and need timely review and advice. Dr Pant has regular weekly lists and can accommodate urgent surgery should that be the best course of action.