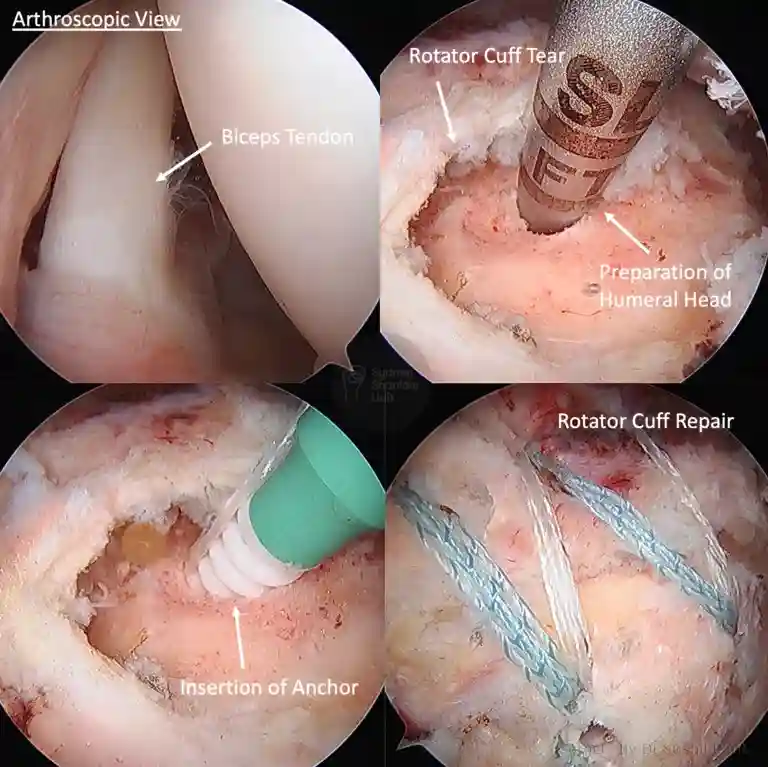
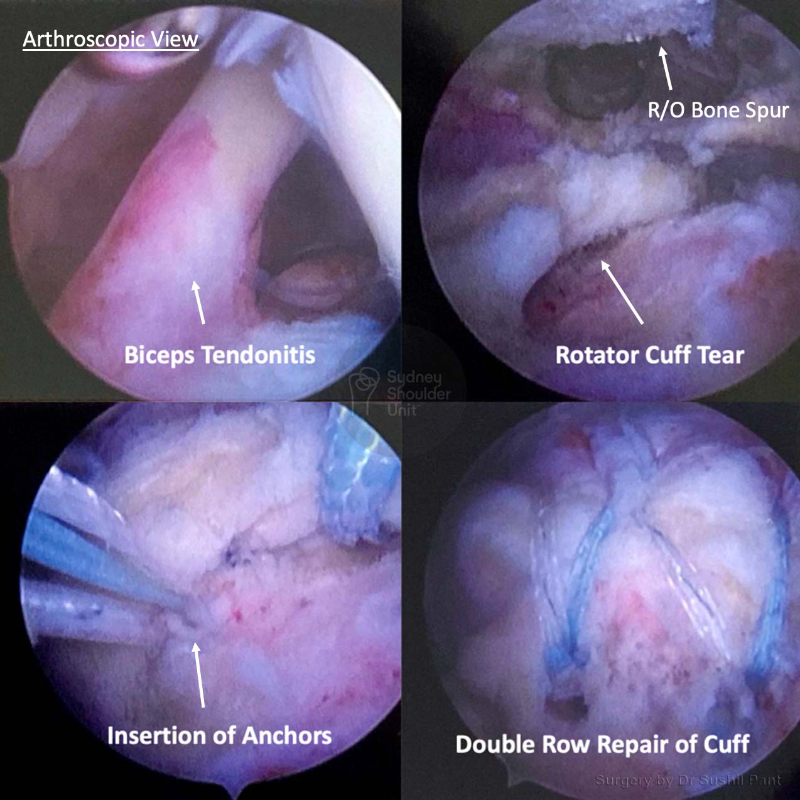
The most common symptoms of a rotator cuff tear include:
- Pain at rest and at night, especially when lying on the affected shoulder
- Pain with lifting or lowering your arm or with specific movements
- Weakness when lifting or rotating your arm
- Clicking for catching sensation when moving your shoulder in certain positions
Generally speaking, acute tears (from a fall or trauma) usually cause intense pain. Some patients report a snapping sensation followed by immediate shoulder weakness.
Tears that develop slowly over time due to overuse may also eventually lead to shoulder pain and arm weakness. Patients may report shoulder or arm pain when lifting the arm, and this pain may move down the arm. Initially, the pain may be mild and only with activity; over time the pain may occur at rest and even at night – waking patients up from sleep and making it difficult to sleep on the affected side. In the initial stages painkillers, activity modification, therapy may settle the symptoms. As the condition progresses, the symptoms persist despite maximising treatment.
Some rotator cuff tears are not painful and may present with weakness and/or loss of function.
Examination
Rotator cuff tears may occur in isolation or with other conditions in the shoulder. A careful history will provide initial clues to other possible diagnoses. The examination focuses on identifying areas of tenderness on palpation – in particular the acromioclavicular joint, biceps tendon, glenohumeral joint (shoulder joint), and the subacromial space (area directly above the tendon). It is important to carefully assess the range of motion about the shoulder joint. Each of the rotator cuff tendons should be carefully examined for integrity and power. Special tests then are used to isolate areas of concern to identify all relevant conditions that coexist.
In some cases, there may be an overlapping syndrome from a “pinched” nerve in the neck that can refer to pain to the shoulder.
Imaging
X-ray: this is the first test to be performed and provides an overall assessment of the shoulder joint; it may show evidence of acromioclavicular joint arthritis, bone spurs, rotator cuff insertion problems, and shoulder joint arthritis.
Ultrasound: this is an easy test to obtain and can be useful; however this test is often very much dependent on the person performing the scan to identify areas of concern.
MRI: This is the most valuable scan when investigating possible rotator cuff tendon conditions. It shows the soft tissues, tendons, muscles, bursa, and shoulder joint in great detail. The rotator cuff tear location, size, muscle quality, tendon quality, degree of retraction can all be assessed with high accuracy. It will also allow assessment of the bursa, shoulder spur, biceps tendon, acromioclavicular joint and shoulder joints in detail.
Assessment of the muscle/tendon quality will help in deciding whether this is a “new” or “old” tear and what treatment options are suitable.